stem cell
Top stories
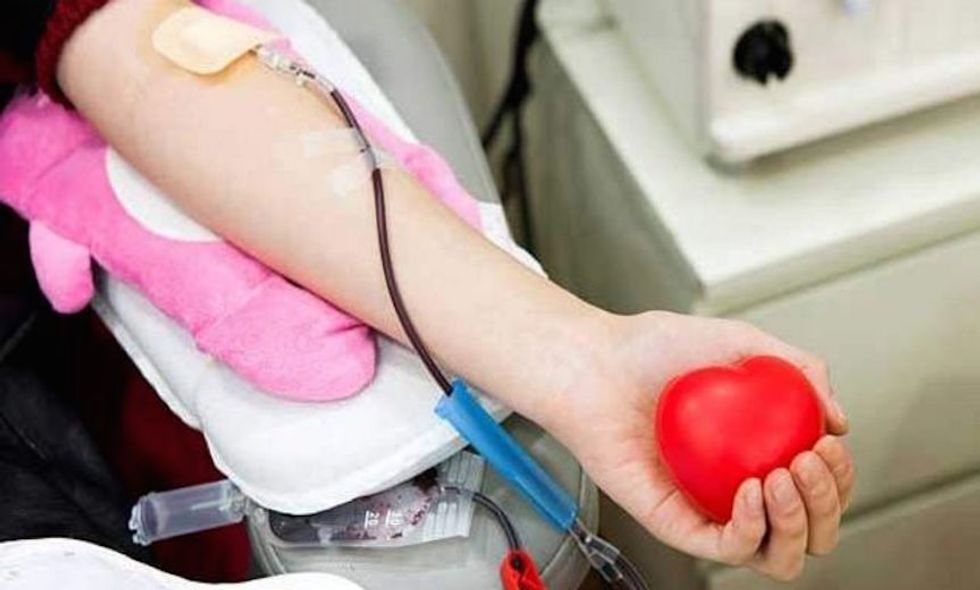
“Immortal” Cells May Bring an End to Blood Donation
Scientists successfully mass produce red blood cells from immortal stem cells
[DIGEST: IFLS, Science Alert, BBC]
Every two seconds, someone in the United States needs blood, with nearly 21 million blood components transfused each year. This demand is hard to keep up with, and the medical community has long been trying to find a way to artificially meet the demand without relying exclusively on volunteers.
A team of researchers from the University of Bristol and NHS Blood and Transport may have done just that, manufacturing red blood cells on a mass scale. The results were published in the journal Nature Communicationslate last month.
While red blood cells have been artificially manufactured before, they have only been produced in very small quantities. The old method worked by taking stem cells, and then turning them into red blood cells. This could produce about 50,000 cells before the stem cells died. To put this in perspective, a typical bag of blood requires 1 trillion red blood cells.

The Bristol team overcame the inefficiency by creating a line of immortal erythroid (or red-blood-cell- producing) stem cells. By trapping the adult stem cells in an early stage of development, the cells can divide and create red blood cells indefinitely.
“We have demonstrated a feasible way to sustainably manufacture red cells for clinical use. We’ve grown liters of it,” said Dr. Jan Frayne, one of the researchers.
Continuing Challenges
While the method is effective, lab-grown red blood cells are still much more expensive than donated blood, and technology does not yet exist to produce the blood on a mass scale.
“To produce that much at scale is quite a challenge, and really the next phase of our work is to look at methods of expanding the yield,” said Professor David Anstee, one of the researchers on the team.
The researchers expect that this method will be useful, though, for people with very rare blood types.
“The first therapeutic use of a cultured red cell product is likely to be for patients with rare blood groups, because suitable conventional red blood cell donations can be difficult to source,” said Anstee.
“The patients who stand to potentially benefit most are those with complex life-limiting conditions like sickle cell disease and thalassemia, which can require multiple transfusions of well-matched blood. The intention is not to replace blood donation but provide specialist treatment for specific patient groups,” Anstee continued.
Clinically developing red blood cells could also be useful in areas where blood supplies are inadequate or unsafe.

“Globally, there is a need for an alternative red cell product,” said Frayne. “Cultured red blood cells have advantages over donor blood, such as reduced risk of infectious disease transmission.”
Clinical trials are expected to begin by the end of the year, and will use manufactured red blood cells from stem cells in an otherwise normal blood donation.
 SECONDNEXUS
SECONDNEXUS percolately
percolately georgetakei
georgetakei comicsands
comicsands George's Reads
George's Reads